Long recognized as a leading cause of death, pneumonia has been studied intensively since the late 1800s. Despite this research and the development of antimicrobial agents, pneumonia remains a leading cause of complications and death.
Pneumonia
Community-acquired pneumonia (CAP) is a syndrome in which acute infection of the lungs develops in people who have not recently been hospitalized and have not been admitted to a nursing home or in centers where elderly patients live. Any other type.
Pneumonia is an infection of the lungs. It is also called pneumonia or bronchopneumonia.
It is a severe disease that can affect people of any age. Still, it is most dangerous in young children, people over 65, and those with underlying medical problems, such as heart disease, diabetes, and chronic obstructive pulmonary disease.
It is more common during the winter months in smokers and men.
Nearly four million cases of CAP occur each year in the United States, and approximately 20% of people with CAP require hospitalization.
How does pneumonia affect breathing?
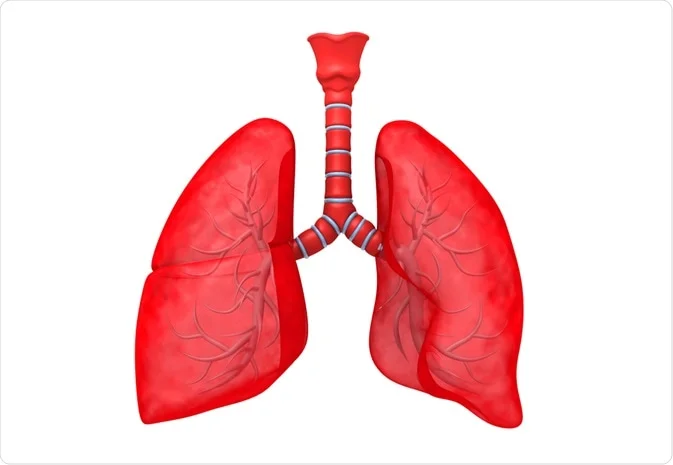
During normal breathing, the air is inhaled through the nose, mouth, trachea, and bronchi to the bronchioles. The bronchioles end in small air sacs, the alveoli. These sacs have thin, porous walls that contain tiny blood vessels called capillaries. This is where gas exchange takes place.
Standard respiratory tree and pneumonia
The mouth and respiratory tree are constantly exposed to microorganisms as air is inhaled through the nose and mouth. However, the body’s defenses are usually able to prevent microorganisms from entering the most profound parts and reaching the lungs. These defenses include the immune system, the anatomy of the nose and pharynx (which helps trap microorganisms and airborne particles from going any further), the ability to cough, and delicate hair-like structures called cilia. , which are located in the cells of the bronchi.
Pneumonia appears if the defenses are inadequate, if one is exposed to an exceptionally healthy microorganism, or if one is exposed to many organisms.
As the microorganisms multiply, the immune system responds by sending white blood cells (leukocytes) to the alveoli. Infected alveoli become inflamed (filled with white blood cells, protein, fluid, and red blood cells). These acute changes lead to the symptoms of pneumonia.
Pneumonia can be caused by various microorganisms, including viruses, bacteria, and, less frequently, fungi.
The most common cause of pneumonia is the bacteria Streptococcus pneumoniae (also called pneumococcus). Other bacteria that lead to pneumonia include Haemophilus influenzae, Legionella pneumophila, and Staphylococcus aureus. Mycoplasma, which commonly causes mild pneumonia, can sometimes cause more severe illness.
Viruses are responsible for less than 20% of adult CAP cases. The flu is a common cause of viral pneumonia.
Fungi rarely cause pneumonia in healthy people; people with a weakened immune system (HIV positive, organ transplant recipients, and those receiving chemotherapy) are at increased risk of fungal infection.
Tell your doctor if you have recently traveled or lived in an area where certain types of pneumonia are more common (for example, valley fever or coccidioidomycosis in the southwestern United States or Middle East respiratory syndrome). In the Arabian Peninsula).
The risk of pneumonia caused by new microbes, the so-called “emerging pathogens,” changes over time. Or, the doctor must know if you have recently been in any places that may pose a greater risk of contagion by any of these emerging germs.
What happens to me when I have pneumonia?
The most common symptoms of pneumonia are fever, chills, shortness of breath, pain with breathing, increased heart rate and breathing rate, nausea, vomiting, diarrhea, and cough that is often accompanied by green or yellow sputum; occasionally, the sputum may be rust-colored.
Most people have a fever (temperature greater than 38°C), although pneumonia in the elderly sometimes occurs without fever.
Chills and a change in mental status, such as confusion or fuzzy thinking, may also occur.
When the doctor thinks of pneumonia…
Pneumonia is usually diagnosed with a complete medical history, physical examination, and chest x-ray.
The need for further testing depends on the severity of the disease and the person’s risk of complications.
chest x-ray
Chest x-ray or sometimes another imaging test, such as a computed tomography (CT) scan, is used to diagnose pneumonia when the history and physical examination also support the diagnosis.
sputum culture
Sputum culture requires a sputum sample obtained from a deep cough. It is used to identify the bacteria that cause pneumonia and can help determine which antibiotic is best.
Urine antigen test
A urinalysis allows, by determining the antigen of some bacteria, the diagnosis of pneumonia caused by two bacteria, Streptococcus pneumoniae and Legionella pneumophila. This test is easy to perform and provides quick results.
Blood test
Hospitalized patients require blood tests, including a complete blood count and sometimes a blood culture (blood culture). The total blood count measures the number of various types of blood cells, including white blood cells (leukocytes); these cells can increase in number when there is a bacterial infection. It also serves as a marker of response to the treatment.
Blood culture is used when the infection is suspected of spreading from the lungs into the bloodstream. It involves taking a blood sample from a vein and culturing it in enriched media in the laboratory to obtain bacterial growth. Under normal conditions, there should be no bacteria in the bloodstream. Blood cultures allow the bacteria that have caused pneumonia to be identified and guide the choice of antibiotic.
Blood oxygen measurement
Pneumonia can decrease the amount of oxygen available in the blood. The oxygen level in the blood is often measured indirectly by attaching a small clip to the finger or ear using infrared light (pulse oximeter). In those who are sicker, the oxygen level is measured by analyzing a blood sample from an artery (arterial blood gases).
bronchoscopy
Patients who present with severe pneumonia do not improve or worsen during hospitalization despite antibiotic treatment and may require additional tests, such as bronchoscopy.
In this procedure, the doctor uses a thin, flexible tube with a camera to view the trachea and bronchi. This allows direct viewing of the innermost part of the respiratory tree, sampling of deep mucus, or even biopsy to determine if there is an underlying cause of the infection, such as an abnormal tissue growth or an inhaled foreign body.
Pneumonia Treatment
The goal of treatment for patients with CAP is to treat the infection and prevent complications.
The initial treatment of CAP is based on the organism that may be causing pneumonia, called empiric treatment. Most patients improve with empirical treatment.
Do I need hospitalization?
Most patients receive oral antibiotic treatment at home. People who are seriously ill or at higher risk of complications are often hospitalized.
The hospital monitors heart and respiratory rates, temperature, and oxygen levels. Hospitalized patients generally receive intravenous antibiotics during the first days of hospital admission.
The number of days the patient requires hospitalization is variable and depends on how they respond to treatment and if there are underlying medical problems.
The choice of antibiotic
We have a series of antibiotic treatment guidelines for the treatment of CAP. The choice of antibiotic