«Dry Eye or Tear Film Dysfunctional Syndrome is the most frequent problem in Ophthalmology, although fortunately, it is only sometimes the most serious.»
The concept of dry eye has changed throughout history. (1) In the time of Hippocrates, the term Xerophthalmia (in Greek, dry eye) was applied only to those who had an absolute dryness of the ocular surface with corneal blindness. (2) Approximately a century ago, new terms appeared to designate certain situations of the ocular surface in which more or less ocular dryness was sometimes detected and that were named for the most differentiating symptoms and signs, such as punctate keratitis, filiform keratitis, keratopathy filamentosa, keratitis sicca, and keratoconjunctivitis sicca. In the last two-thirds of the last century, it was assumed that most dry eyes were Sjögren’s syndromes, whose meaning also changed over the years, and the other etiologies were underestimated or ignored. (3) About half a century ago, von Rötth introduced the term Dry Eye for any lacrimal gland insufficiency, a concept that was gradually completed with those of water deficiency, lipodeficiency, and immunodeficiency. (4) Currently, some dacryologists think that the term Dry Eye should also be extended to qualitative deficiencies (deficiency of lysozyme, taurine, growth factors, etc.)
As the general population currently understands the term Dry Eye, its use has become widespread and accepted, despite not being very academic, and has become what linguists call a “lexical solidarity,” that is, a combination of two or more terms, where the association means something other than the two terms separately. However, it is important to know that Dry-Eye lexical solidarity can be used with four different meanings: as a symptom, as a sign, as a syndrome, and as a disease. As a “symptom,” it is the subjective sensation of dryness (although occasionally there is no dryness). As a “sign,” it is the objective decrease in tear secretion. As a “syndrome,” it is the association of ocular dryness with its concomitant manifestations (foreign body sensation, photophobia, conjunctival vasodilation, fissure blepharospasm), although the causes that produce the syndrome are different from one case to another. As a “disease,” it is each of the many clinical pictures of different etiologies and nosologies (menopause, autoimmune endocrinopathy, vitamin A deficiency, etc.) in which the dry eye syndrome is an important manifestation, in addition to the different manifestations according to the etiological cause. Looking for a parallel with fever, the symptom is the sensation of fever; the sign, hyperthermia; the syndrome, hyperthermia with its typical associations of malaise, loss of appetite, tremor, mental confusion, etc .; and the disease, the various diseases of different etiologies, associated with fever such as yellow, foot-and-mouth, Maltese, quartan, rheumatic fever, etc. When the doctor talks with other colleagues or his patients, he must be aware of all these possibilities.
Dry Eye? Stop suffering
What is dry eye?
Dry eye syndrome is caused by a lack of lubrication and moisture on the surface of the eye. It can cause considerable discomfort and lead to problems ranging from mild eye irritation to severe chronic inflammation if left untreated. If not diagnosed and treated promptly, dry eye syndrome can lead to scarring on the front of the eye.
It is a very common problem affecting about half of the population, especially after 50 years of age.
Dry eye, symptoms
The patient may have the following dry eye symptoms:
The feeling of dry eyes
Itchy eyes
Sensation of pain
Heaviness in the eyelids
Eye fatigue
Blurry vision
Annoyance with bright lights or photophobia
Eye redness
Foreign body sensation, like sandAs the disease progresses, and if it is not treated, the eye can become inflamed, causing pain, redness, and finally damage to the ocular surface that can be irreversible.
Eye damaged by severe dry eyes
Dry eye causes
To begin to explain the causes, it is important to mention that tears are composed of various substances and that the tear must be adequate to keep the eyes moist and eliminate substances that can damage them or cause infections, such as dust and some microorganisms. A suitable tear must contain a compaqueous component (water), an oil component (lipids), and a mucous component (mucin). Each of these components is produced by different glands found in the eye and on the eyelids.
In this way, the malfunction in any of these glands causes the tear to be inadequate, and the eye is not humidified and protected properly.
Among the causes or factors related to dry eye are:
Excessive sun exposure
Prolonged exposure to dry environments (wind, dust, air conditioning, or heating)
Consumption of tobacco products
Consumption of certain medications
Heat or chemical burns
Surgeries
Eyelid problems
Aging
Wearing contact lenses
Autoimmune diseases (such as Sjörgren's syndrome, diabetes, thyroid problems, among others)Dry eye, diagnosis
As various factors can cause dry eye, a thorough review by an eye health specialist, such as an ophthalmologist, is essential. The ophthalmologist must perform a complete study of the eye and its function. This checkup includes an exam of the eye, the lids, and the surface of the eye. In addition, the specialist can perform a test to measure the quality, thickness, and quantity of tears produced by the eye.
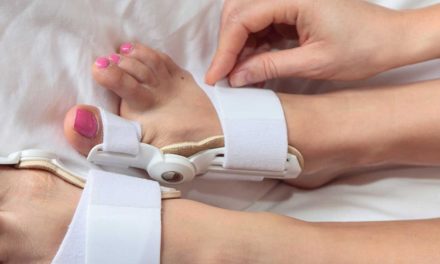
The ophthalmologist may perform a study known as the Schirmer test to confirm the diagnosis and see if the eye produces enough tears to maintain adequate moisture. In this test, the specialist first places anesthetic drops in both eyes and then inserts the tip of a special strip into the lower eyelid of each eye. He will ask you to keep your eyes closed for 5 minutes without rubbing or squeezing your eyelids. After this time, the doctor removes the strip of paper and measures how much it got wet.
Application of drops or artificial tears for dry eye
Dry eye, treatment
The first of the remedies for dry eye is prevention, so the patient is advised to avoid the factors that lead to this syndrome, such as exposure to dry environments, smoke, or excessive heat.
In addition to prevention, another essential step in treating dry eye syndrome is the application of dry eye drops, also known as artificial tears. These drops have components very similar to those of the eye’s natural tears and can be applied as often as the patient prefers to maintain adequate moisturization of the eye. Sometimes these tears can cause allergies due to the preservatives they contain. However, there are preservative-free options for these particular cases.
Depending on the damage and the specific cause, the ophthalmologist may prescribe special medications as a treatment for dry eye to decrease the inflammation of the eye, stimulate the production of tears, or treat the specific disease-causing this syndrome. It is important to understand that the dry eye medication your doctor prescribes should be administered as prescribed by your ophthalmologist. Some medications are sold exclusively by prescription and cannot be administered for a long time or cannot be stopped overnight.
Dry eye, application of drops as a treatment for dry eyes
Dry eye, tear plug placement.
In some cases, the ophthalmologist may opt for a simple procedure where small plugs are placed in the tear ducts. These points are small holes in the tear drainage system found on the inside of the upper and lower eyelids. By plugging these holes, the tears are not drained and remain intact for longer on the surface of the eye, relieving symptoms.