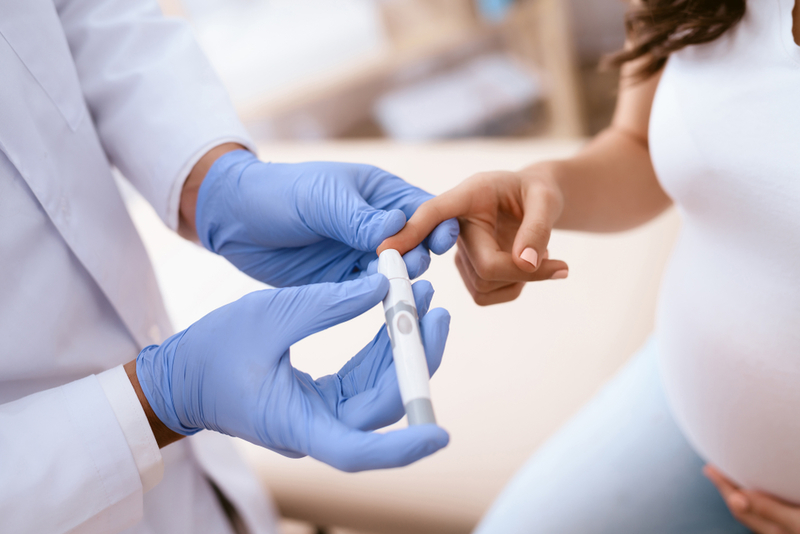
The Apgar test is the first assessment that is made to the baby at birth; since 1952, an obstetric anesthetist from the United States, Dr. Virginia Apgar, began to apply a method to know the adaptation and vitality, of newborns, to the change from the womb to the outside, in this way it is established whether or not there is a need for immediate medical care.
Thanks to Dr. Apgar’s test, many babies have saved their lives by being able to detect prematurely any problem that, if not seen, could be fatal within minutes or hours after delivery.
It is fast because if there is a problem, you have to act as soon as possible, and it does not bother you because if everything is normal, it is not necessary to make the baby feel bad at a time of evaluation.
The Apgar test is done twice to see the baby’s evolution: one minute after birth and five minutes later. It is a scale with which the baby’s heart rate, breathing, muscle tone, reflexes, and color are observed.
The test is divided into five sections or questions that score from 0 to 2. Once done, the points are added, which in most cases is 8 to 10 points in the first minute of life. If that moment, the Apgar is 5 to 7, it may be due to oxygen supply problems during labor, and then the professionals will apply a nearby source of oxygen and probably dry it with a towel relatively vigorously to motivate the baby to breathe harder. With both interventions, the score should be 8 to 10 at 5 minutes.
In 1952, Dr. Virginia Apgar presented a new method for evaluating the newborn, and the following year she published her test under the title “A Proposal for a New Method for Evaluation of the Newborn Infant.” From that moment, every newborn, anywhere in the world, is subjected to the Apgar test at birth.
The score generated by this test is an essential prognosis in the vitality of the newborn, so it is responsible for assessing the response of the newborn to extrauterine exposure. The first evaluation is carried out one minute after birth, then 5-10 minutes after birth.
In the first minute, the baby’s tolerance at birth is evaluated, and in minute five, the evolution of the baby outside the mother’s womb. This test takes into account in its assessment:
Heart rate: if the heart rate is not found, if it is weak (less than 100bpm) or fast (more significant than 100bpm).
Respiratory effort: if the newborn is breathing or has respiratory distress, her crying is loud.
Muscle tone: if you have body movement and do not have mobility, find your legs and arms bent and resist the extension.
Irritability or reflexes: if the newborn responds to stimuli, he cries weakly or loudly.
The skin color: if the baby is yellow (jaundice), blue (cyanotic), or pink.The score ranges from 0 to 7; the higher the score, the better the state and evolution of the newborn; if the score is less than seven, this baby must be constantly monitored to monitor her condition.
Interpretation of the Apgar test
Classification to the minute:
Apgar of 7-10: Normal child (gral. 7-9)
Apgar score 4-6: Mild to moderate asphyxia.
0-3 Apgar: Severe suffocation
Classification at 5 minutes:
- Apgar from 0-6: Extrauterine maladaptation
- Apgar score of 7 or +: Good extrauterine adaptation
What can be the causes of a low Apgar score?
Some of the conditions that can cause a low Apgar test are: Umbilical cord problems: due to a circular cord in the newborn’s neck.
Detachment of the placenta: part of the membrane is detached from the uterus.
Uterine rupture: when there is a tear in the wall of the uterus.
Trauma to the newborn’s head caused by the instruments used in childbirth, the baby’s poor position during the birthing process (breech or face presentation), giant babies (macrosomia), very narrow pelvis for the newborn’s size, shoulder dystocia (baby’s shoulder gets stuck in mom’s pelvic bone)
Preeclampsia
Hypoxia / Asphyxia
What pathologies can arise after a difficult delivery?
Infant Cerebral Palsy: it is a sequel resulting from a non-progressive encephalopathy in an immature brain, whose cause can be pre, peri, or postnatal. It is characterized by alterations of the neuromuscular, skeletal muscle, and sensory systems. In mild cases, most children with cerebral palsy can be identified by the age of 6 months if appropriate developmental assessments, developmental histories, medical follow-up is used and listened carefully to what parents report.
Brachial Plexus Palsy: it is a nerve injury caused by the overstretching of the baby’s neck and shoulders to one side, which generates the partial or total rupture of the brachial plexus; this causes loss of sensation and muscular control of the shoulder, arm, forearm, hand, and finger, according to the level of injury.
These injuries and others are addressed at FisioClinics Madrid by our physiotherapists specialized in the children’s area, who perform adequate and personalized rehabilitation work to treat injuries or pathologies.
Comprehensive family care instruments offer a graphic and schematic appreciation of the family and its relationships; it allows to development of an integrated vision of current interactions, the strengths and weaknesses of the family, and its historical development. They are an essential element diagnostic for the family doctor.
They promote the interest or expression of feelings between the informant, the patient, and the health professional, allowing the understanding of the environment and the context of their family to seek the best way of help that can be provided to the person as a whole.
It allows identifying the extent to which the family fulfills its essential functions and what role family functionality may be playing in the health-disease process, which is why they represent essential elements in first-level outpatient practice and primary care for patients. General health.
The instruments that the family doctor has at his disposal are extensive and must be used according to the needs of the patient and the environment that the specialist detects in the daily consultation. Among the most used instruments, we have the: Family APGAR, Genogram, Ecomap, and the Family File. This time we will refer specifically to the first.
WHAT IS FAMILY APGAR?
The family APGAR is an instrument that shows how family members perceive the level of functioning of the family unit globally, including children, since it applies to the child population.