What is the Apgar test?
This test is named after Virginia Apgar, an anesthesiologist specializing in obstetrics, who devised the test in 1952 at Columbia University Hospital.
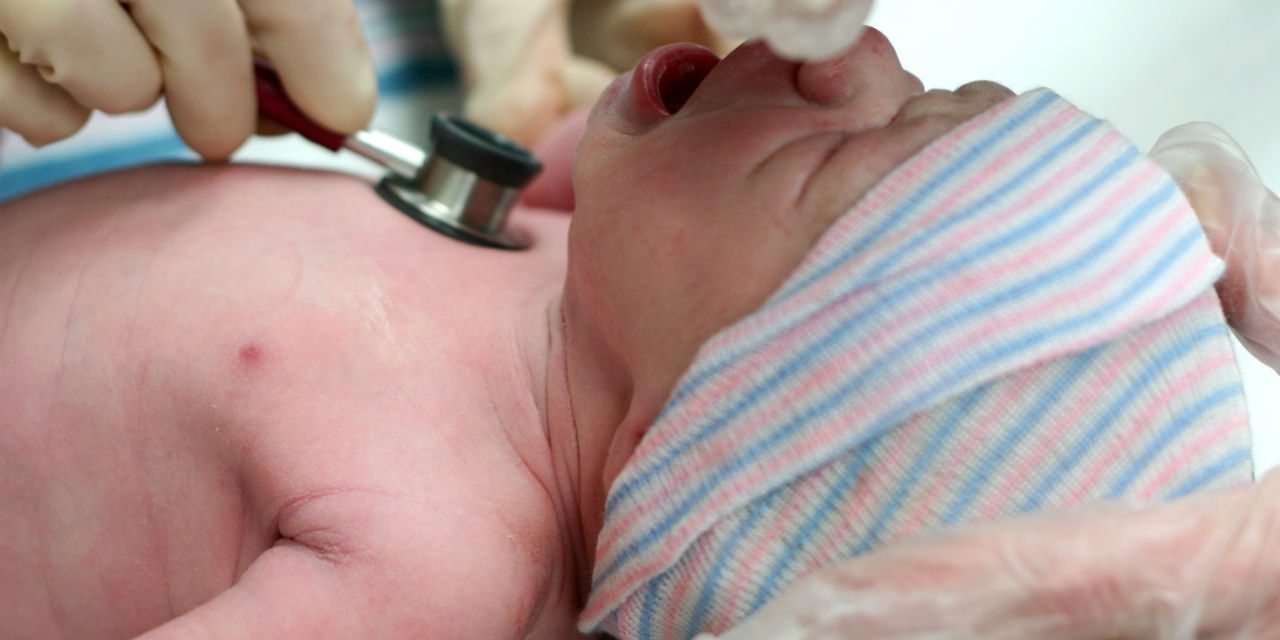
The Apgar test is a test that is carried out when the baby is born to assess its status. It is done at minute 1, at 5, sometimes it is also practiced at minute 10. During the first minute, the baby’s tolerance to the process of being born and whether there has been suffering is measured. At 5 minutes, the adaptation of the newborn to the environment is examined.
Five parameters are taken into account:
– your heart rate
– The reflections
– the color of his skin
– your breathing
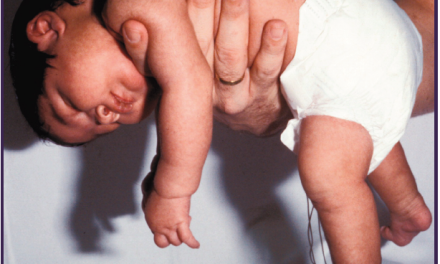
– muscle tone
Each parameter is given a score from 0 to 2. If the sum reaches 7, everything is normal.
What is the Apgar test? Relationship with medical negligence
The Apgar test is a test to assess the condition of the baby after birth.
It is used to determine if the newborn needs additional or emergency medical help.
What does the Apgar test evaluate?
Shortcuts
This test takes into account five factors that are considered essential for the baby’s health. The initials of these dots give the test its name.
Appearance: Regarding the color of the skin. If you notice bluish areas or have a typical hue.
Pulse: Heart rate is checked. Greater or less than 100 beats per minute
Irritability: It is the child’s reflex response. In English, the word is ‘Grimace.’
Activity: State of muscle tone.
Breathing: It measures the respiratory rhythm and if respiratory effort is made.
These factors are scored with a 2, 1, and 0. The 2 is the highest score and reflects normality. Instead, the 0 represents the absence of that factor, and it is more worrying.
To calculate the total, the scores of the different factors are added. The maximum that can be achieved is 10. If the baby scores 7 points or more, it is considered normal. A lower score may mean that the newborn needs some immediate medical treatment.
The test is repeated 5 minutes later. If the evaluation is low and does not improve or the health workers assess that the condition is inadequate, the baby will be treated.
How does it relate to medical malpractice?
In cases of medical negligence, this indicator indicates that the child at birth did not have normal conditions.
Whether it was due to hypoxia before or during delivery, a lack of well-being monitor that went unnoticed, or malpractice at the time of birth, the newborn shows values below normal.
To do this, he developed a method that allowed him to quickly and easily assess the viability of the newborn. The Apgar test was first published in the July-August 1953 issue of the journal Current Researchers in Anesthesia and Analgesia under the title “A Proposal for a New Method of Evaluation of the Newborn Infant.” – the elegance and simplicity of the study increase the admiration of those who read it – and immediately it began to be used in all maternity wards.
The Apgar test reduced neonatal mortality and laid the foundations for modern neonatology. In the words of Apgar herself, what she wanted with her method was a simple and precise classification of the condition of newborns to be able to compare the results of different obstetric practices, analgesic regimens, and newborn resuscitation.
The history of the Apgar test
Virginia Apgar, who died in 1974, continues to give “her look” to all children born in any maternity ward in the world. Her method is straightforward and is the first thing a pediatric resident learns when caring for newborns in the delivery room.
In the 30s of the twentieth century, in the United States, most deliveries were in hospitals. Despite this, infant mortality was higher than in Europe, where childbirth took place mainly at home. Dr. Apgar realized that most children died from lack of oxygen (anoxia) and detected that this was mainly due to 3 situations: maternal anesthesia (which also sedated the child), the lack of training of the doctor who cared for the newborn (often a novice resident) and the lack of consensus about “normal” in the newborn.
Knowing the status of the fetus before birth was challenging, fetal monitors did not exist, but at the time of birth, the problems were evident to simple clinical observation. And this obviousness interested Apgar so much that she got the anesthesia residents at her hospital, the Presbyterian in New York, to begin mandatory rotations in obstetrics. Children who were not breathing, who were pale, who had bradycardia, who were not active, received the appropriate cardiopulmonary resuscitation (CPR) techniques.
Apgar test form with clock
On one occasion, a resident asked Apgar: “How can we make a quick assessment of the newborn’s situation?” Apgar took a piece of paper and replied: “Easy, do it like this, rate these parameters: 1. heart rate, 2. respiration, 3. muscle tone or activity, 4. reflex response to stimulation, 5. color.”
The Apgar test was born.
Dr. Apgar spent a whole year developing a scoring system that allowed her not only to determine the need to apply CPR maneuvers but also to establish a basis for comparison and discussion of obstetric procedures, types of maternal anesthesia, and the results of resuscitation.
The studies carried out by Apgar, and her colleagues served as the basis for a better understanding of the physiology of the newborn and many aspects of maternal-fetal metabolism unknown in her time. Her method became widespread throughout the world and has dramatically improved the survival and health of newborns.
The first thing the baby does as it is born is to go through the Apgar test. It is an evaluation that is carried out in two phases and that allows the health workers who are attending the birth to know first-hand the vital situation in which the child is in the extrauterine world.
How the Apgar test was created
Dr. Virgina Apgar created this test in 1952. She wanted to objectively define how suffocation had affected a newborn at the time of delivery, and she used the parameters commonly used by anesthetists to determine the degree of anesthetic depth. From that moment on, the Apgar test was consolidated and currently, as pointed out by Dr. Manuel Sánchez Luna, president of the Spanish Society of Neonatology (SENEO), integrated into the AEP (Spanish Association of Pediatrics), “continues having validity and also represents an international language. “
The importance of the test goes in two ways: “Its objective is not only to know the state of the newborn at birth, but its response to resuscitation maneuvers when they are necessary,” says the neonatologist. This is essential, as it allows doctors to make the most appropriate decisions at a critical moment when the child may be at risk due to different circumstances.